Is the COVID-19 Vaccine Safe?
Featured Experts:
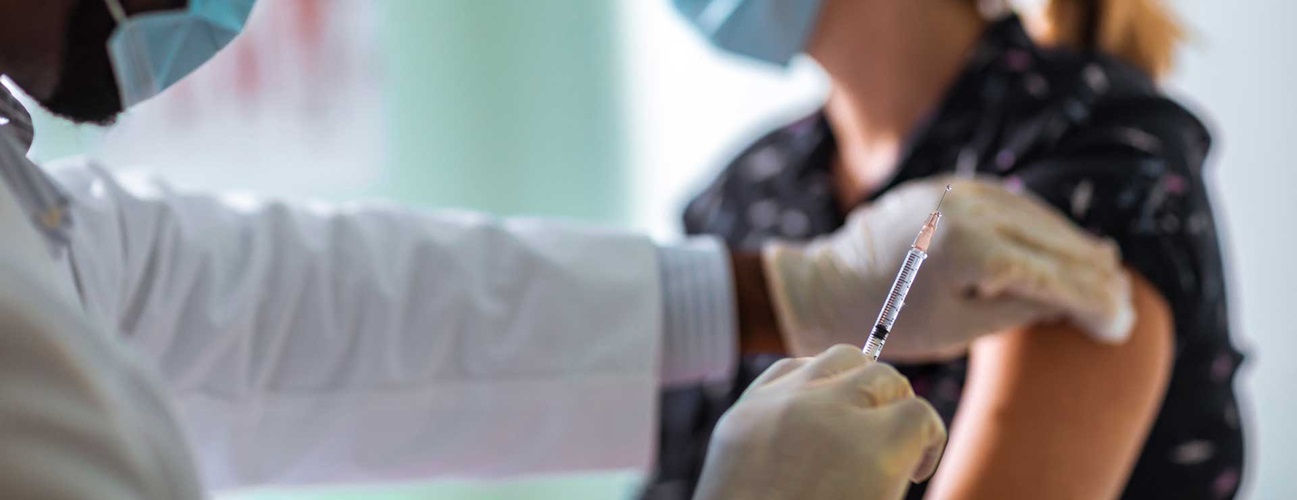
The arrival of the first COVID-19 vaccines is a major development in the coronavirus pandemic. An effective COVID-19 vaccine will help protect people who come in contact with the virus from becoming sick. As more people are vaccinated, families and communities will be able to gradually return to a more normal routine.
Some people are asking if the COVID-19 vaccines are safe. Lisa Maragakis, M.D., M.P.H., senior director of infection prevention, and Gabor Kelen, M.D., director of the Johns Hopkins Office of Critical Event Preparedness and Response, answer questions you might have as you consider getting a COVID-19 vaccine.
Is the COVID-19 vaccine safe? What do we know about its safety?
The U.S. vaccine safety system works to make sure that all vaccines are as safe as possible. Safety has been a top priority as federal agencies work with vaccine manufacturers to develop and authorize a COVID-19 vaccine. Here are some key areas that are part of a COVID-19 vaccine development, review and authorization:
- Careful testing. All vaccines go through clinical trials to test safety and effectiveness. For the COVID-19 vaccine, the Food and Drug Administration (FDA) set up rigorous standards for vaccine developers to meet. This infographic from the National Institutes of Health shows the four phases a vaccine must go through before it is released to the public.
- Authorization for emergency use. Vaccines that meet FDA safety and effectiveness standards can be made available in the United States by approval or by emergency use authorization (EUA). An EUA provides temporary authorization of a vaccine or medication under emergency situations, such as the coronavirus pandemic.
- Continuous monitoring for problems and side effects. Once a vaccine is authorized for use, monitoring continues, with systems in place to track problems or side effects that were not detected during the clinical trials. For the COVID-19 vaccine, the FDA and the Centers for Disease Control and Prevention (CDC) are expanding their vaccine monitoring. If there are problems with the vaccine, they are most likely to emerge early in the testing process when they can be identified and addressed.
You can learn more from the CDC about the safety steps in place for the COVID-19 vaccine.
Have there been any safety concerns with the COVID-19 vaccine?
So far, none of the vaccine trials have reported any serious safety concerns. Trials for the first two vaccines — from Pfizer and Moderna — have had fully independent safety monitoring boards, and safety data are continuously reviewed by the FDA and expert panels.
Allergies: The CDC says people with allergies to certain foods, insects, latex and other common allergens can have the COVID-19 vaccine. Those with a history of severe allergic reaction (anaphylaxis) to injectables or other vaccines should discuss the vaccination with their doctor, who can evaluate the person and assess their risk. According to the CDC, at this time, anyone who has a severe allergy (e.g., anaphylaxis) to any of the Pfizer/BioNTech vaccine ingredients should not receive this vaccine.
How Do We Know a COVID-19 Vaccine Will Be Safe and Effective?
How was the COVID-19 vaccine developed so quickly?
In the past, vaccines have taken many years to develop. However, the relatively quick development of this vaccine does not mean safety measures were skipped. There are several reasons why the COVID-19 vaccines were developed faster than other vaccines:
- The mRNA technology used to develop the COVID-19 vaccines has been years in development to prepare for outbreaks of infectious viruses. Thus, the manufacturing process was ready very early in the pandemic.
- China shared genetic information about the SARS-CoV-2 coronavirus when it was available, which gave vaccine developers an early start at finding a vaccine.
- The testing processes for the vaccines didn’t skip any steps, but the vaccine developers conducted some stages of the process simultaneously to gather as much data as quickly as possible.
- Governments gave money to vaccine developers in advance, so the companies had resources they needed.
- Some types of COVID-19 vaccines were created using messenger RNA (mRNA), a new technology that allows a faster approach than the traditional way vaccines are made.
- Social media enabled companies to reach out to and enroll study volunteers, and plenty of people wanted to help, so there were enough research participants to test the COVID-19 vaccines.
- Because the SARS-CoV-2 coronavirus is so contagious and widespread, many volunteers who got the vaccine were exposed to the virus, and with so many exposures, the trials took a shorter time to see if the vaccine worked.
- Companies began manufacturing vaccines ahead of their authorization or approval so some supplies would be ready if authorization occurred.
How effective are COVID-19 vaccines?
Pfizer’s vaccine was authorized on Dec. 12, 2020, and Moderna’s version is being reviewed by the FDA. Both manufacturers report that their vaccines show approximately 95% efficacy at preventing both mild and severe symptoms of COVID-19. This level of efficacy appears to apply across age groups, racial and ethnic groups, and both sexes, as reported in the Pfizer trial.
Why is it Important that I Consider Getting the COVID-19 Vaccine?
Will I still have to wear a mask and continue COVID-19 safety precautions if I get the vaccine?
Yes, everyone still needs to maintain these safety precautions for the foreseeable future. If you are among the estimated 5% to 10% of people for whom the vaccine is not effective, you could still catch and spread the coronavirus. Studies are looking at whether the vaccine, even when effective at preventing disease, keeps a person from harboring the virus and passing it to others.
What are the side effects of the COVID-19 vaccine?
Vaccine developers report side effects that include pain at the injection site, fever, muscle aches, fatigue and headaches, mostly lasting about a day or two. If symptoms persist, you should call your doctor.
If you have allergies, especially severe ones that require you to carry an EpiPen, discuss the COVID-19 vaccine with your doctor, who can assess your risk and provide more information on if and how you can get vaccinated safely.
Can I get COVID-19 from the vaccine?
You cannot get COVID-19 from the vaccine. The COVID-19 vaccines created by Pfizer and Moderna do not have any virus or other infectious material in them. They are designed to cause your body to make copies of a harmless piece of the coronavirus, so you will not get COVID-19 from the vaccine. Side effects such as fever and soreness at the injection site have been reported, particularly after the second injection (both of these vaccines require a second injection three to four weeks later), but the reported COVID-19 vaccine side effects in the trials are not as severe or dangerous as having a bad case of COVID-19 illness.
What about safety of the COVID-19 vaccination for diverse groups of people?
The FDA and other reviewers closely consider diverse populations included in the trials for safety purposes. The clinical trials for the first two COVID-19 vaccines included underrepresented minorities (about 25% of participants), older age groups (about 25%), and people with conditions such as obesity, diabetes and heart and respiratory conditions.
Note: The trials did not include pregnant women or children under 12. Trials with these groups are in progress or are scheduled to begin soon.
Demographics of the COVID-19 Vaccine Trials
Does Johns Hopkins Medicine recommend I get a COVID-19 vaccine?
You alone make the decision about whether to get a COVID-19 vaccine. We encourage you to talk to your primary care doctor and review our resources provided here, as well as information from other health care organizations. Johns Hopkins Medicine will continue to provide science-based, unbiased information so you can make an informed decision.
Coronavirus (COVID-19) Email Alerts
Sign up to receive coronavirus (COVID-19) email updates from Johns Hopkins Medicine.What is messenger RNA technology?
The first two COVID-19 vaccines were created using a new technique called messenger RNA, or mRNA. The method has been in development for years before the pandemic, and the arrival of the new coronavirus provided vaccine manufacturers a chance to use it.
Vaccines against viruses work by sending a message to the body to be on the lookout for a certain virus, such as SARS-CoV-2. Traditional approaches have used dead or weakened versions of the virus itself, which the body learns to identify and develop immunity to. Making new vaccines this way can take years.
The mRNA approach works differently. When a virus such as SARS-CoV-2 enters the body, it sets in motion a means of producing copies of itself like a photocopy machine. The copies of the virus invade other cells. The mRNA coronavirus vaccines cause the body to produce copies of just one part of the coronavirus: the spike proteins on its surface that give the virus its telltale appearance. The spike protein helps the virus attach to cells and make people sick, but by itself, cannot cause COVID-19.
The new mRNA vaccines for the coronavirus contain “instructions” for how to make copies of the spike protein. The mRNA is synthetically made in a lab (meaning it is not taken from the virus directly). It is manufactured to be injected and to find its way into cells. In the cell, mRNA instructs the cell to make copies of the coronavirus’s spike proteins. When the cell releases these proteins, the immune system identifies them as foreign and destroys them, but not before making antibodies to detect and react to the protein and the virus that causes COVID-19. Then, later, if a live, complete coronavirus enters the person’s body, the immune system “remembers” the spike protein and attacks the coronavirus so it cannot reproduce and make someone sick with COVID-19.
Vaccines created with mRNA may be even better at protecting people from disease than those made with dead or weakened viruses.